This Is How Much Women With Endometriosis Are Spending Just To Function
Companies, agencies, institutions, etc
Ubers
National Action Plan
Medicare Benefits Schedule
BuzzFeed News
GP
IVF
Doherty
decade.“Then
Hennessy
Dunlevie
the Pharmaceutical Benefits Scheme
uterus.“[My
physiotherapist.“Even
infusion.“Because
HomeSitemap
People
Greg Hunt
Syl Freedman
Gemma Cafarella
Doherty
Lacee Hennessy’s
Imogen Dunlevie’s
Zelesski
Emily Zelesski
issues.“When
right.”Zelesski
Gina Rushton
Groups
Australians
Endometriosis
Physical locations
No matching tags
Places
EndoActive
Locations
Melbourne
parents’
GP
urologist.“The
Sydney
Inc.
Events
the Sydney Morning Herald
Summary
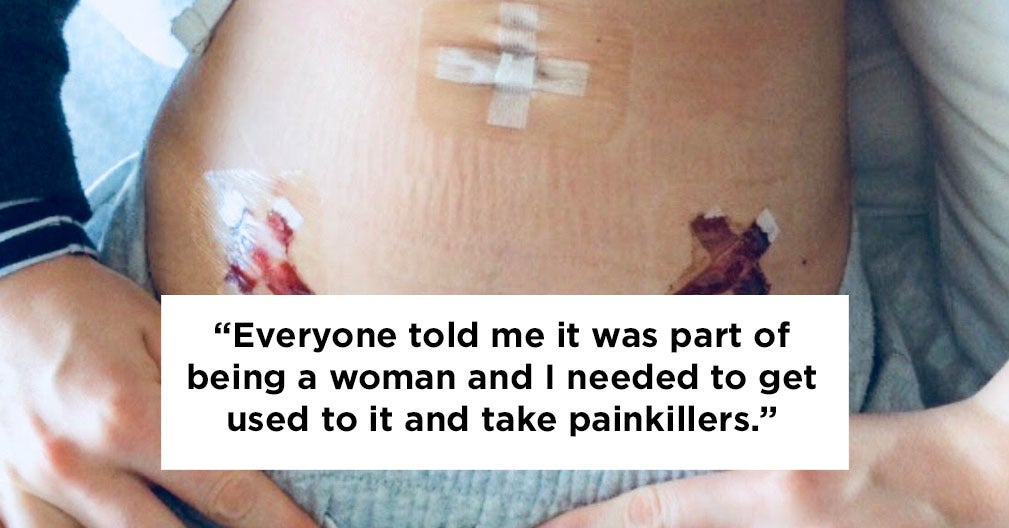
The disease can lead to debilitating long-term chronic pain, compromised fertility and sexual dysfunction.The federal government’s National Action Plan for Endometriosis, released in July last year, acknowledges endometriosis is “chronic”, “common”, “frequently under-recognised” and that it impacts the “social and economic participation, physiological, mental and psychosocial health of those affected”.The plan refers to research that indicates the condition could be more common than breast cancer and diabetes for women aged 15 to 49 and costs Australian society $7.7 billion each year — two-thirds from lost productivity and the rest from direct healthcare costs.There’s a debate among clinicians and those living with endometriosis as to whether the government’s Medicare Benefits Schedule (MBS) review, specifically recommendations made by its gynaecology committee, would increase the costs of laparoscopies, which are crucial to diagnosing and treating the condition.Private gynaecologists told the Sydney Morning Herald the cost of the operation could increase by as much as 20%, but a spokesperson for health minister Greg Hunt told BuzzFeed News the government was “always looking to do more for women affected by endometriosis” and that the minister would have more to say on this “in the very near future”.“The government would not under any circumstances contemplate higher out of pocket costs and nor do we see the committee as recommending that,” the spokesperson said.Co-founder of health promotion charity EndoActive, Syl Freedman, was on the steering committee for the national plan and said any cost increase would be “awful for patients”.“We really hope that any recommendations by the [MBS] review committee won’t incur extra costs for endo patients,” Freedman told BuzzFeed News.“It is very, very expensive to live with a chronic illness and taking out the obvious costs of surgery and prescriptions and over the counter medication and pain relief, there are complementary therapies so things like pelvic floor physio, acupuncture, seeing a naturopath or dietician or gastroenterologist.”Freedman, who lives with endometriosis, said there were also costs associated with loss of productivity.“We already know that there are people with endo who are on the disability pension because they can’t work,” she said. “The existing costs of living with a chronic illness is a devastating burden for women with endometriosis and their families and any additional costs could really make or break a situation for a lot of people.”BuzzFeed News spoke to five women about what they spend to manage their endometriosis.It took a decade of pain and an emergency surgery before Melbourne lawyer Gemma Cafarella was finally diagnosed with a condition she long believed she had.“I had complained of endometriosis-like pain since I was 18 to GPs and I wasn’t actually diagnosed until I was hospitalised for burst ovarian cysts when I was 28,” the now 31-year-old told BuzzFeed News.“They did it all at once and removed the endometriosis and a couple of cysts so when I woke up I found out that I’d been formally diagnosed.“For 10 years I’d been saying I could have endometriosis but was told my period cycle wasn’t consistent with someone who had endo, which I now know to be completely irrelevant, so by the time the [cysts burst] I was in around the clock pain.”Cafarella sees her GP on average once a month, a private gynaecologist multiple times a year and a range of private specialists to treat complications caused by her endometriosis.She occasionally sees a specialist gynaecologist physiotherapist where the initial session was $170 and the subsequent sessions are $120.“The recommendation is that I do a course of six or eight sessions and these have no rebates, it is all privately paid for,” she said.Cafarella has also seen a gastroenterologist for $170 due to complications from her first surgery: “I was then diagnosed with a potential bladder complication where one urologist thinks the endometriosis is actually growing outside of my bladder.”When Cafarella sought a second opinion from another urologist, she was told she needed $1,500 worth of treatment for interstitial cystitis, a chronic bladder condition.“He laughed when I asked if there were any [public system] options,” she said.She does not have private health insurance and believes in universal healthcare.“I want to pay the additional tax and I want that to be put into the healthcare system and I want to be contributing for other people who can’t afford to,” she said.Any increase in the the cost of laparoscopy would be “gutting”, she said.“The laparoscopy was free and I can’t tell you how grateful I was that it was free,” she said. A cream for pelvic pain is about $200, with no rebate.She is currently casually employed while studying so getting sick is “very expensive”.“I know I’ve gone to work when I definitely don’t feel well enough to be there, because the cost is too much to miss out on.”Emily Zelesski.Nurse Emily Zelesski has always had painful periods.“Everyone told me it was part of being a woman and I needed to get used to it and take painkillers,” the 26-year-old told BuzzFeed News.When Zelesski was 19 she was sent for an ultrasound, told she had polycystic ovaries and put on the oral contraceptive pill, which she eventually came off for cardiac issues.“When I came off it I had the worst period pain I’ve ever had in my life and it got to the point where I was getting pain every single day, outside of my period cycle,” she said.
As said here by Gina Rushton